Gestational Diabetes and Everything About It
Key Highlights
- Gestational diabetes is a highly prevalent global problem that affects the health of both, the mother and child.
- Though the causes are not well understood, gestational diabetes mainly affects women who are overweight/obese, have a history of GDM, suffer from PCOS, or are older.
- Diagnosis can be performed using tests like glucose challenge test/ oral glucose tolerance test.
- Managing GDM involves lifestyle changes, including diet and exercise, monitoring blood sugar levels, and medication.
- By taking proper precautions and care, GDM can be prevented, and even if you have been diagnosed with GDM, further complications can be prevented.
- With appropriate steps, the mother and the child can live a healthy life after childbirth.
Are you a mother-to-be? If yes, congratulations, you are in for a wonderful ride! These nine months will be truly transformative for you. Your maternal instincts might start to kick in right from the time of conception. Which is how you tend to be extra careful, taking every precaution to ensure your child's safety. This includes being warned and aware of complications like gestational diabetes and being aware of gestational diabetes menu ideas to tackle the condition if need be.
But first, we need to understand what exactly is gestational diabetes? Let's take a closer look.
Diabetes and its types
Diabetes, or specifically diabetes mellitus, is a disorder where the processing of sugar in the body is hampered. This affects how the food we eat is converted into energy.
Insulin is a hormone that allows blood sugar to enter the cells to produce energy. The levels of the hormone insulin are affected in this disorder.
Diabetes may be essentially classified into 3 types:
- Type 1 Diabetes: The body does not produce insulin in Type 1 diabetes. This condition is usually present since birth and may also be referred to as juvenile diabetes.
- Type 2 Diabetes: The body produces insulin, but fails to utilize it properly. It commonly affects obese individuals.
- Gestational diabetes: This type of diabetes onsets during pregnancy.
What is gestational diabetes?
Gestational diabetes is a type of diabetes that develops during pregnancy. It develops in women who don't already have diabetes. Like other types of diabetes, gestational diabetes also affects how your body utilizes sugar.
Excess sugar in the blood during pregnancy is not good for you or your baby's health. Gestational diabetes is more common than you think, which is why you need to be watchful of your sugar levels during pregnancy.
Insulin production during gestational diabetes

Gestational diabetes is similar to type 2 diabetes in that the body does produce insulin; however, the cells are not able to utilize it. Your pancreas works overtime to produce insulin, however, this insulin cannot effectively lower your blood sugar levels, thus making you diabetic during your pregnancy.
Facts about gestational diabetes
As we said, gestational diabetes is more common than you think. So if you are suspected of having gestational diabetes, worry not. You aren't alone.
- 20 million women had some form of hyperglycemia in pregnancy. An estimated 84% were due to gestational diabetes.
- Approximately 50% of women with a history of GDM go on to develop type 2 diabetes within five to ten years after delivery.
- 1 in 6 births is affected by gestational diabetes.
- The vast majority of the global burden of gestational diabetes comes from low- and middle-income countries. This could be credited to the lack of access to sufficient maternal care in these countries.
These statistics also make it clear that gestational diabetes is an important issue that pregnant women need to be aware of and take necessary actions to prevent and control gestational diabetes.
Problems caused during pregnancy
If your blood sugar is not under control, then gestational diabetes can cause the following complications:
1. High blood pressure (Preeclampsia)
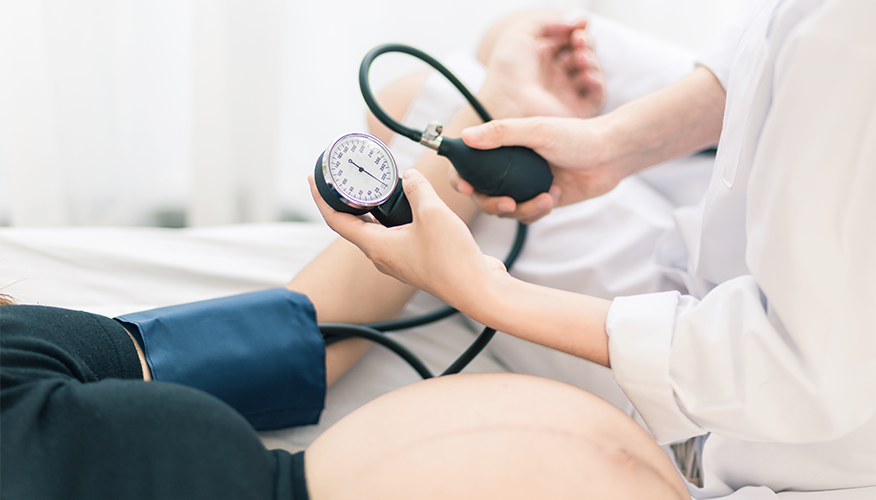
A pregnant woman may have preeclampsia if:
- High blood pressure,
- Protein in her urine, and
- Swelling in fingers and toes that does not go away.
2. C-section
A pregnant woman may have preeclampsia if:
- A C-section or Cesarean section is an operation performed to deliver the baby through the mother's belly.
- If diabetes is not well controlled during pregnancy, there is a higher chance of needing a C-section for delivery.
- If a C-section is performed to deliver the baby, it takes longer for the mother to recover from childbirth.
How does it affect your baby?
Glucose is a nutrient that can cross the placenta. So if you have gestational diabetes, extra blood glucose goes through the placenta, giving the baby high blood glucose levels. The baby's pancreas thus produces more insulin.
This can cause the following problems:
1. Overfed/Extra-large baby:
Since the excess insulin produces excess energy in the baby's body, it gets stored as fat. This can result in macrosomia or a "fat baby". Macrosomia can result in health problems down the line, during adulthood. An extra-large baby is difficult to carry in the womb for the mother. It can also cause damage to the baby's shoulder during bir
2. Low blood sugar
If gestational diabetes is not well controlled during pregnancy, the baby can very quickly develop low blood sugar after birth. The baby's blood sugar must be watched for several hours after delivery.
Since gestational diabetes develops at a relatively later stage in the pregnancy, after the development of many of the baby's body parts, it does not cause the kinds of birth defects seen in women with diabetes before pregnancy.
What causes gestational diabetes?
The exact cause of gestational diabetes is still not understood well. However, it is attributed to the hormonal changes that occur during pregnancy. The placenta is an organ formed during pregnancy to support the baby's growth. Hormones from the placenta help the baby grow.
However, these hormones also disturb the action of insulin in the mother's body, causing her to develop something called insulin resistance, which makes it difficult for her to utilize the insulin produced. She may need up to 3 times more insulin as a result.
Gestational diabetes risk factors

Are you wondering about your risk of developing gestational diabetes during pregnancy?
Here are some risk factors to help you estimate the same:
- Had gestational diabetes during a previous pregnancy
- Have given birth to a baby who weighed more than 9 pounds
- Are overweight/obese
- Are older than 25 years
- Have a family history of type 2 diabetes
- Have a polycystic ovary syndrome (PCOS), a hormonal disorder
What are the symptoms?
There are no clear symptoms that you may experience than those of a normal pregnancy. You may feel thirstier than usual. You may also find that you are urinating more than usual. Irrespective of these symptoms, a proper diagnosis is required to ascertain if you have gestational diabetes.
Tests and diagnosis
Your healthcare provider can help you diagnose gestational diabetes with some clinical tests. The timeline of testing is a crucial part of the diagnosis.
1. When to get tested?
If you have an average risk of gestational diabetes, your healthcare provider may suggest screening during your second trimester, sometime around 24-28 weeks of pregnancy.
However, if you are at high risk(as suggested by the risk factors above), your doctor may recommend getting screened during your initial visits when you first get pregnant.
2. Screening and diagnostic tests
Your doctor may employ certain blood tests to diagnose gestational diabetes. They may employ one or more tests to ascertain the diagnosis. Most doctors might follow the two-step approach.
The tests used for diagnoses include:
1. Glucose Challenge Tes
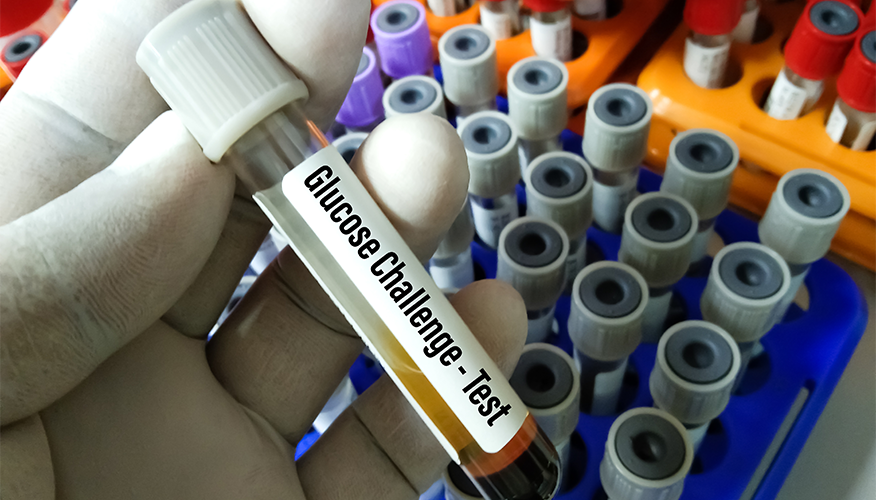
- This test is also called the glucose screening test. Your doctor might recommend this test first.
- You do not need to fast for this test.
- The healthcare professional will ask you to drink a sweet liquid containing glucose and draw your blood 1 hour later.
- If your blood glucose is >140, your doctor might ask you to return for the oral glucose tolerance test.
- If your blood glucose is >200, you might have type 2 diabetes.
2. Oral Glucose Tolerance Test (OGTT)
- This test is also called the glucose screening test. Your doctor might recommend this test first.
- You do not need to fast for this test.
- The healthcare professional will ask you to drink a sweet liquid containing glucose and draw your blood 1 hour later.
- If your blood glucose is >140, your doctor might ask you to return for the oral glucose tolerance test.
- If your blood glucose is >200, you might have type 2 diabetes.
Managing gestational diabetes
The basic management of gestational diabetes may be three-pronged. Firstly, you need to implement some lifestyle changes. Second, you need to closely monitor your blood sugar levels. Sometimes, you may require certain medications to correct the condition. Let's look at these three a bit more closely.
Lifestyle changes to manage gestational diabetes
Lifestyle changes mainly include what you eat, i.e. food with health benefits, and how active you are.
1. Diet
A healthy eating plan is crucial during pregnancy, especially if you have gestational diabetes. Being aware of meal and snack ideas for gestational diabetes, and discussing gestational diabetes diet menu ideas for a healthy eating plan, with your healthcare provider are important. Here are some general recommendations and tips for you to look into
- Eat a variety of healthy foods to make a balanced diet.
- Read food labels while shopping for groceries.
- Eat three small- to moderate-sized meals and one or more snacks each day
- Do not skip meals or snacks. Instead, look for meal and snack ideas for gestational diabetes that you can easily make at home
- Keep the amounts of different food groups the same every day to keep your blood sugar stable
- Eat plenty of whole fruits and vegetables, moderate amounts of lean proteins and healthy fats, moderate amounts of whole grains (such as bread, cereal, pasta, and rice), plus starchy vegetables (such as corn and peas), fewer foods that have a lot of sugar (such as soft drinks, fruit juices, and pastries)
2. Exercise

Staying active is important at every stage of women's lives, including pregnancy. Exercise can help in the following ways:
- Lower your blood sugar
- Help relieve some common discomforts of pregnancy, including back pain, muscle cramps, swelling, constipation, and trouble sleeping.
- Achieve normal blood pressure and cholesterol goals in case they are high
- Relieve stress, strengthen your heart and bones, improve muscle strength, and keep your joints flexible
- Lower chances of developing Type 2 Diabetes in the future
Discuss exercise with your doctor and aim for 30 minutes of activity 5 days a week. If you weren't active before pregnancy, no worries, you can build up your stamina and strength gradually.
3. Monitoring blood sugar
Your doctor may ask you to check your blood glucose levels 4 or more times a day. You may be asked to use a blood glucose meter that requires a drop of blood to produce the results. Record the results every time you check your blood glucose. You can record the results in a diary or maintain an electronic record on your phone through an app/ your computer. Make sure you carry these records when you visit your healthcare provider.
Recommended levels at different times are:
- Before meals, at bedtime, and overnight: less than or equal to 95
- 1 hour after eating: less than or equal to 140
- 2 hours after eating: less than or equal to 120
4. Treatment
Sometimes, eating healthy and staying active is not enough. If doing these two as per instructions is also not enough to get your glucose levels in the target range, you may require medical treatment. Your doctor may initiate treatment with insulin. Insulin is not taken orally, hence your healthcare provider will instruct you or your spouse to administer insulin safely. Insulin is the first choice for treating gestational diabetes as it does not harm the child. Researchers are still studying the use of oral diabetes medications such as metformin for use, and have found some success, however, long-term use still needs to be studied and evaluated.
5. Preventing Gestational Diabetes
We have already discussed the potential risk factors that can predispose you to develop gestational diabetes. Some risk factors can not be modified, such as your genetics and family history. However, there might be some things you can do to curb your risk before you try to get pregnant.
If you are overweight or obese, you can try to lose some weight. You can start by exercising regularly. This can help you control your weight and reduce blood sugar levels.
However, it is recommended that you do not try to lose weight once you are pregnant, as you might need to gain some weight to support your baby's growth. Speak with your doctor about how much weight gain and physical activity during pregnancy are right for you.
Did you like our Article?
Excited
0
Happy
0
Not Sure
0
Silly
0
- Diabetes During Pregnancy Available at CDC
- Gestational Diabetes and Pregnancy | CDC Available
- Gestational diabetes - Symptoms and causes - Mayo Clinic Available
- How Gestational Diabetes Can Impact Your Baby Available at Diabetes
- Gestational Diabetes - Symptoms, Treatments | ADA Available
- Tests & Diagnosis for Gestational Diabetes | NIDDK Available
- Screening, Diagnosis, and Management of Gestational Diabetes Mellitus - American Family Physician Available
- Gestational diabetes - Diagnosis and treatment - Mayo Clinic Available
- After Your Baby is Born | NIDDK Available
- Managing & Treating Gestational Diabetes | NIDDK Available
Our team of experts frequently monitors developments in the health and wellness field, and we update our articles when new information becomes available.
Current Version
Mar, 26 2024
Written By
Dr. Kulyk Alexander Petrovich
Aug, 21 2023
Written By
Dr. Kulyk Alexander Petrovich
Leave a Comment